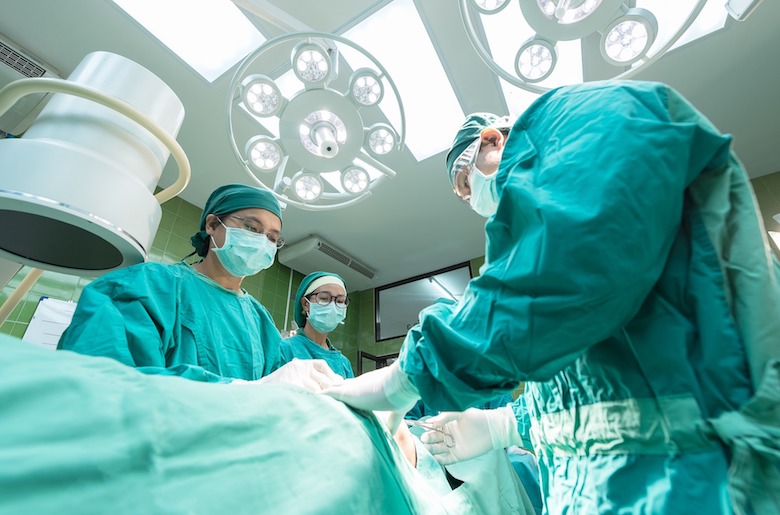
Provider burnout can seriously compromise physician’s careers and mental health — and, just as importantly, the quality and safety of patient care — and still the issue remains. Keep in mind that, as administrative and systemic complexities have increased in the healthcare system so, too, have rates of physician burnout. In fact, a recent study shows that, between 2011 and 2014, physician burnout across all specialties rose from 45% to 54%. Physician burnout can’t be solved by a yoga class, telling physicians to take more time off and have “a better work/life balance,” or ignoring it. This year, let’s resolve to alleviate the systemic burdens that lead to physician burnout.
Make better use of non-physician providers
Non-physician providers such as advanced practice nurses, registered nurses, physician assistants, clinical education specialists and care coordinators can be used to free up doctors to do the actual practice of medicine. Tasks that can be assigned to these providers include triaging patient needs, setting the patient-encounter agenda, double-checking medications, providing discharge-plan education, following up on the care plan at regular intervals, arranging preventive services, exchanging records and notes between physicians on the care team, and the list goes on.
However, proposals to expand the work of these providers have been met with resistance. The concerns of physicians are not without merit, and they need to be involved in the process of creating standing orders, protocols and decision-making pathways for non-physicians to use in their work. When these safeguards are in place, more high-functioning practices are developed, which can result in more daily patient visits and higher revenues that exceed the costs of hiring non-physicians.
Developing non-physician provider programs creates team-based care that supports physician and patient alike. Hiring scribes in particular is one of the key ways to improve physician satisfaction within this context. Taken together, care teams that aid the physician in providing accessible, effective, efficient care often translate to a better work/life balance for physicians.
Provide extra EHR support
Electronic health records (EHRs) are a valuable tool for documentation and communication, and they aren’t going away. However, there is no doubt that trying to combine documentation on clunky interfaces with patient care keeps physicians from doing enough of the latter. For example, a Johns Hopkins study found that interns are spending 12% of their time with patients and more than 40% in front of a computer screen. In addition, a study published in the Annals of Internal Medicine found that physicians spend nearly 50% of their time on EHR and desk work, and just over a quarter of their time with patients. Even in the exam room, physicians spend 37% of their time on EHR and desk work.
Simply put: EHRs are not user-intuitive enough to allow physicians the time to care for patients, which means patient engagement suffers which, in turn, means physicians become frustrated with their workload and lack of satisfaction from their work. Physicians have trained long and hard to become good doctors who provide excellent patient care, not good clerical workers. Clerical work is critical to the functioning of any practice or hospital — but doing both at the same time detracts from interaction with the patient, in-depth information gathering and discussion, and patient education.
When scribes take on real-time data entry, physicians are free to focus solely on the patient. Instead of fiddling with a computer system, the physician is making a diagnosis, ordering tests and medications, and giving the patient information about their condition. That’s the kind of scenario that provides a physician with job satisfaction at the end of the day. In addition, reports a recent Medscape investigation into physician burnout, “[T]he extra person [in the exam room] actually improves the physician-patient relationship because the physician is able to provide his or her full attention to the patient and is not distracted by data entry.”
Engage and empower physicians
Just as patients need to be engaged as part of their care, doctors, too, should be empowered to prevent their own burnout. Only 20% of physicians are fully engaged with the healthcare institutions that hire them — a harbinger of physician burnout. Physician burnout can be expedited when doctors lose the incentive to practice — or, more often, lose the desire to engage with a healthcare system that doesn’t provide them with the means to practice. The drive to lower costs and increase efficiency can sometimes make it seem that medicine is losing sight of patient care.
“The C-suite perspective holds that a lack of control induces burnout. Some executives advocate an approach to addressing burnout that emphasizes physician empowerment rather than coping mechanisms,” writes Modern Healthcare. The journal cites programs working hospitals now, such as a physician leadership academy that helps enhance physicians’ communication and management skills, so that they can better participate in controlling their own work environments.
This kind of control can manifest in healthcare organizations should create physician-led committees to help find practical, low-cost solutions and lead the drive for change without compromising patient care. Engaging physicians in these activities, so they can directly influence care and outcomes, leads to better physician buy-in and higher physician satisfaction with their work. When bolstered by a non-punitive culture of care, hospitals can help fully support physicians who are, after all, human beings first and foremost.